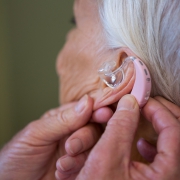
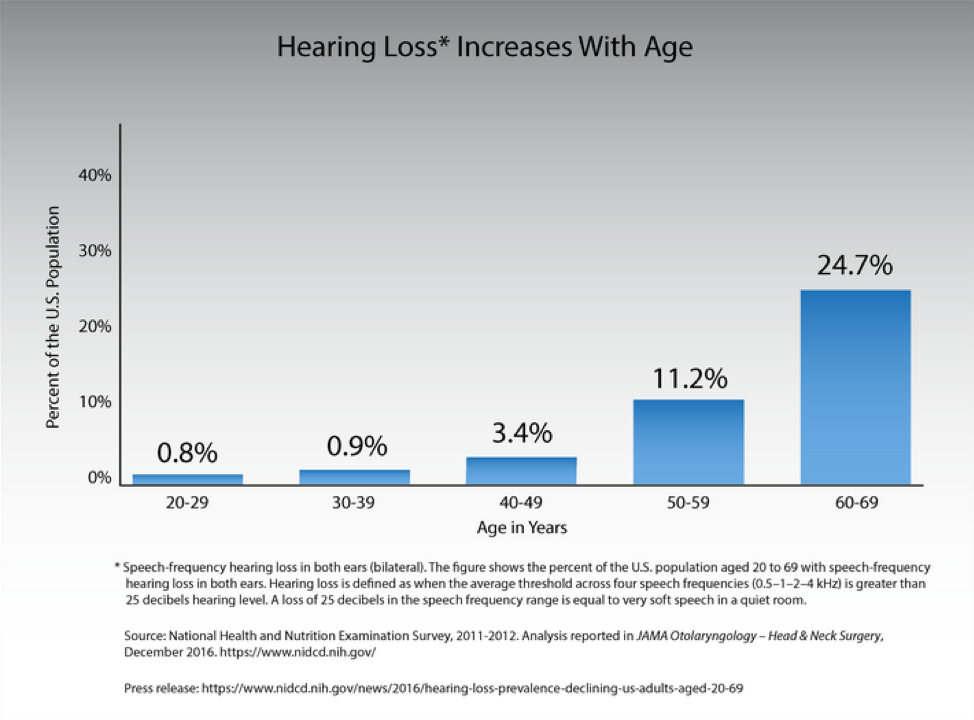
A Nursing Home can be Covered by Medicaid
Remember Medicaid planning doesn’t simply mean meeting strict income and asset limits to qualify for long-term care insurance. You will also need to demonstrate you need the level of care typically provided in a nursing home setting. These health eligibility rules are valid if you apply for nursing home coverage. Or a Medicaid waiver program for coverage in your home. Each state has a level of care requirement. And its own criteria to determine if you meet the mandated level of care. It can get complicated because eligibility criteria are not always clear.
Determining the level of care necessity usually includes:
- The need for two or more activities of daily living constitutes bathing, toileting, dressing, eating, and mobility.
- You require frequent medical care, like IVs or other injections, medications, or other medical treatment.
- You exhibit behavioral problems such as aggressiveness or wandering away from home.
- Alzheimer’s disease or another form of dementia impairs your cognitive ability. Making decisions on your own is problematic and/or you cannot correctly process information.
The state evaluates the assessment of a Medicaid applicant and, in many cases, will require a doctor’s diagnosis. The assessment generally requires the applicant to answer a series of questions about their abilities to perform activities of daily living and any behavioral issues or cognitive problems. There are further questions regarding the applicant’s family and their ability to provide support.
Understanding Medical Services Covered by Medicare
Medicare still covers the medical services you may need beyond nursing care along with institutional Medicaid. If you need to see a specialist or go to a doctor’s office, Medicare pays first, and Medicaid will cover your remaining costs like copayments, coinsurances, and deductibles. When applying for institutional Medicaid, consider the following:
- The program considers you and your spouse together when counting assets and income. Typically, you can set aside a certain amount of assets and income to protect your spouse’s standard of living. This spousal amount does not count when applying for Medicaid.
- You will still be able to keep a small amount of income for your allowance even though you qualify. The amount varies by state, and your local Medicaid office can provide more information. The remainder of your income will pay the nursing home.
- There is a look-back period of up to five years for institutional Medicaid in most states. When determining your eligibility, your state will count any assets you have transferred in the past five years. If Medicaid determines any transfers violate the Medicaid eligibility rules, you may be penalized. Medicaid may opt to pay only a portion of your nursing home stay or none at all.
- Owning your own home affects Medicaid eligibility and coverage. An elder law attorney can characterize your specific circumstances and how the equity in your home may count as an asset. When long-term care is no longer necessary, or you are deceased, these assets may repay Medicaid for your care coverage.
Nursing Home and Assisted Living
Nursing home level of care, also known as nursing facility level of care (NFLOC), Is not an easily definable term as there is no formal federal definition. Each state has the task of defining the term, and rules are not always consistent from one state to the other. Generally, there are four areas of concern, though not every state considers all four; physical functional ability, medical needs/health issues, cognitive impairment, and behavioral problems.
For those families with a loved one who requires more care than they can provide at home but do not require a high enough level of care to qualify for nursing home admittance, there is an in-between care type typically provided in assisted living. However, Medicaid coverage of this type of assisted living is very limited in numbers.
Nursing homes are experiencing very limited capacity, and waitlists can be years. Medicaid is adapting to provide this coverage type in-home to those applicants who may meet NFLOC Medicaid eligibility requirements but not pose a danger to themselves or others in a home environment. Perhaps using this as a springboard as a potential nursing home residence is waitlisted for full-time care.
Getting Informed
Before applying to become eligible for Medicaid nursing home coverage, there is much to consider. Applications that are insufficient or incorrectly filed can create delays, and with limited space available, it can be several years on a waiting list before admittance can take place.
The need is more significant than ever before for long-term care in a nursing home. Meeting your state’s eligibility requirements can be a long and complex series of providing documents, answering questionnaires, having assessments and reviews, and filling out and filing forms. The scope of the project can be overwhelming. To get to your best outcome, don’t wait. Contact our Ruston, LA office today at (318) 255-1760. Proactive planning with an elder law attorney will help you understand and address all criteria you need to act on to succeed.